4 Dermatological Applications of Mesenchymal Stem Cell-Conditioned Medium (MSC-CM)
- Oct 15, 2025
- 5 min read
As dermatology advances into the regenerative medicine era, mesenchymal stem cell-conditioned medium (MSC-CM) has emerged as a game-changing tool, offering a cell-free, bioactive solution to some of the field’s most persistent challenges. A comprehensive review by Zare, S., Jafarzadeh, A., Zare, S. et al. (2025) synthesizes recent clinical findings on MSC-CM and its diverse dermatological applications—from reversing skin aging to restoring hair growth, accelerating wound healing, and repairing acne and surgical scars.
What is MSC-CM?
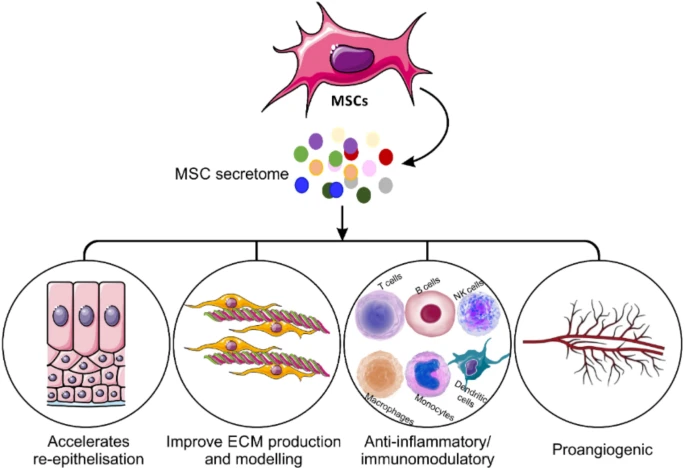
Mesenchymal stem cells (MSCs) are multipotent stromal cells found in bone marrow, adipose tissue, umbilical cord, and other organs. Rather than using the cells themselves, MSC-CM refers to the secreted “conditioned medium” rich in growth factors, cytokines, exosomes, and extracellular matrix proteins.
Key components of MSC-CM include:
VEGF: Promotes angiogenesis
bFGF & HGF: Stimulate fibroblast activity
IGF-1 & KGF: Enhance epithelial regeneration
PDGF: Drives fibroblast proliferation and matrix remodeling
These act through paracrine signaling—modulating tissue repair, immune response, and dermal regeneration without the complexities of direct stem cell implantation.
4 Dermatological Applications of Mesenchymal Stem Cell-Conditioned Medium (MSC-CM)
1. Wound Healing
Mechanism of Action
The MSC secretome accelerates wound healing primarily through paracrine signaling, where secreted growth factors such as VEGF, EGF, FGF, and TGF-β play pivotal roles. These bioactive molecules enhance keratinocyte proliferation and migration, stimulate angiogenesis, and modulate fibroblast activity for efficient extracellular matrix remodeling. Furthermore, exosomes in the secretome carry microRNAs (miRNAs) that regulate genes involved in the inflammatory and proliferative phases of wound healing, promoting faster closure and tissue regeneration.
Clinical Evidence
Multiple in vivo and in vitro studies have supported the secretome’s efficacy in cutaneous wound repair. A murine study demonstrated significantly accelerated epithelialization and collagen deposition in wounds treated with human MSC-derived secretome. In a small-scale clinical pilot, topical application of conditioned media from adipose-derived stem cells (ADSCs) reduced healing time in chronic ulcers without adverse events, suggesting a favorable safety and efficacy profile.
Clinical Application
In clinical settings, the MSC secretome is typically delivered via topical formulations, such as hydrogels or creams containing conditioned media, or through microneedling-assisted delivery to enhance penetration. It is increasingly integrated into post-laser recovery protocols, pressure ulcer treatment, and diabetic wound care regimens. Its acellular nature makes it suitable for repeated applications without eliciting immune responses, a crucial advantage in chronic wound patients.
2. Photoaging and Skin Rejuvenation

Mechanism of Action
The rejuvenating effect of the MSC secretome on photoaged skin is mediated by the upregulation of collagen and elastin synthesis and downregulation of matrix metalloproteinases (MMPs), which are responsible for dermal matrix degradation. TGF-β and IGF-1 in the secretome enhance fibroblast activity, promoting dermal thickening, while antioxidants and anti-inflammatory cytokines reduce oxidative stress and UV-induced inflammation.
Clinical Evidence
Histological analysis from clinical trials has shown increased dermal density and improved collagen fiber arrangement in subjects treated with ADSC-conditioned media. A double-blind, placebo-controlled trial involving topical application of ADSC-CM for 4 weeks revealed visible improvement in skin elasticity, hydration, and wrinkle depth. These findings corroborate the regenerative signaling cascade triggered by the secretome in aged dermis.
Clinical Application
Secretome-based cosmeceuticals are now being used in anti-aging skincare lines and in post-procedural care following fractional CO₂ laser or RF microneedling. Dermatologists may also incorporate MSC secretome into injectables or mesotherapy solutions to enhance skin quality in the periorbital and malar regions. Its compatibility with adjunctive treatments like PRP and botulinum toxin expands its utility in holistic facial rejuvenation protocols.
3. Hair Regeneration

Mechanism of Action
Hair follicle stem cell activity and dermal papilla cell survival are central to hair growth, both of which are positively influenced by the MSC secretome. Key growth factors like PDGF, IGF-1, and VEGF stimulate anagen phase entry, improve follicular vascularity, and delay apoptosis of hair matrix keratinocytes. Exosomal miRNAs further support follicular regeneration by modulating Wnt/β-catenin and Sonic Hedgehog (Shh) signaling pathways.
Clinical Evidence
Recent randomized controlled trials have demonstrated improved hair density and thickness in androgenetic alopecia patients treated with exosome-rich MSC secretome injections. In one study, a 12-week course of biweekly secretome injections led to a 29% increase in hair density compared to placebo. Preclinical studies also show enhanced follicular neogenesis in murine alopecia models when exposed to MSC-derived exosomes.
Clinical Application
The secretome is commonly delivered via intralesional microinjections or mesotherapy guns across the scalp, typically in combination with microneedling. It is often used as an adjunct or alternative to minoxidil and finasteride, particularly in patients who seek non-pharmacologic interventions or experience side effects from oral medications. The treatment is repeated every 2–4 weeks over several sessions to sustain follicular stimulation.
4. Inflammatory Skin Diseases (e.g., Atopic Dermatitis, Psoriasis)

Mechanism of Action
In the context of inflammatory skin diseases, the MSC secretome acts as a potent immunomodulator. It downregulates pro-inflammatory cytokines such as IL-6, TNF-α, and IL-17 while upregulating anti-inflammatory mediators like IL-10 and TGF-β. Additionally, exosomes from MSCs modulate the behavior of T cells, dendritic cells, and macrophages, rebalancing the immune response and reducing chronic inflammation in skin lesions.
Clinical Evidence
Preclinical studies have shown reduced epidermal hyperplasia and decreased inflammatory infiltrates in psoriasis and AD animal models after secretome application. A Phase I clinical study evaluating the topical use of MSC-conditioned media in mild-to-moderate atopic dermatitis reported marked symptom improvement and reduced need for topical corticosteroids. The reduction in Th2-mediated cytokine production has been particularly significant in these trials.
Clinical Application
Secretome-based topical formulations are being trialed as steroid-sparing agents in chronic inflammatory skin conditions. They are used in conjunction with basic emollient therapy and, in some cases, as part of personalized compounded skincare under dermatologic supervision. As systemic delivery of stem cells or immunosuppressants can carry risks, topical or localized secretome delivery offers a safer, targeted alternative.
Benefits of MSC-CM Over Traditional Treatments
Feature | Traditional Therapy | MSC-CM |
Mechanism | Direct targeting | Paracrine modulation & regeneration |
Invasiveness | Often surgical/injection | Topical or minimally invasive |
Immunogenicity | Moderate (e.g., PRP autologous) & May vary (especially in allogeneic sources) | Low (cell-free, acellular) |
Risk of Hyperpigmentation | Present in lasers | Reduced when combined with MSC-CM |
Downtime | Variable | Shortened recovery time |
Repeat Treatments | Often needed | Enhanced outcomes with fewer sessions |
Infection risk | Minimal | Higher in live cell-based or invasive therapies |
Storage & shelf-life | Requires cryopreservation or live handling | Stable (lyophilized or frozen) |
Standardization | Cell-based variability | Easier to standardize |
Regulatory pathway | Complex in cell-based products | More favorable (non-cellular) |
Limitations
Standardization Needed: MSC-CM lacks uniform manufacturing protocols (source, concentration, preservation).
Regulatory Oversight: While safer than live-cell therapy, CM use still falls under regulatory scrutiny in many countries.
Limited Long-Term Data: Most studies are <6 months follow-up; more longitudinal studies are needed.
Adjunctive Use Preferred: MSC-CM shows the best results when combined with microneedling, lasers, or RF.
Conclusion
MSC secretome represents a paradigm shift in dermatologic therapy, moving beyond symptom control toward cellular-level tissue restoration. Its multifaceted action—regenerative, anti-inflammatory, angiogenic—makes it a valuable adjunct or alternative in managing conditions ranging from aging and alopecia to chronic wounds and inflammatory dermatoses. As clinical evidence continues to grow, dermatologists and aesthetic physicians are likely to find increasing opportunities to integrate MSC-based therapies into daily practice.
Reference:
Zare, S., Jafarzadeh, A., Zare, S. et al. Exploring the dermatological applications of human mesenchymal stem cell secretome: a comprehensive review. Stem Cell Res Ther 16, 177 (2025). https://doi.org/10.1186/s13287-025-04311-8
Learn techniques behind Stem Cell Therapy
in our upcoming Mini Fellowship:
IFAAS Mini Fellowship (Observational)
Anti-Aging Stem Cell Therapy: Japan Edition
Anti-Aging Stem Cell Therapy: Japan Edition - Tokyo, Japan - [Register Now]
Anti-Aging Stem Cell Therapy - Seoul, South Korea - [Register Now]
More Upcoming Global Events








Comments